Periodontal disease represents one of the most widespread pathological conditions in small- animal practice, affecting the vast majority of dogs and cats by early adulthood (80% of dogs and cats by age of 3 years) [9].
The chronic, progressive nature and capacity to inflict both local and systemic harm make periodontal disease a central concern in veterinary medicine. The gold-standard approach to treatment is grounded in a clear understanding of the disease’s pathophysiology, the diagnostic tools required for accurate assessment, and the therapeutic interventions proven to halt progression and restore oral comfort.
Contemporary veterinary guidelines, particularly the American Animal Hospital Association (AAHA) Dental Care Guidelines for Dogs and Cats, provide the most authoritative framework for managing this condition in clinical practice [1].
Understanding the Pathophysiology of Periodontal Disease
Periodontal disease begins with the formation of a bacterial biofilm on the tooth surface. This biofilm, commonly referred to as plaque, develops within hours after a tooth is cleaned and consists of a complex microbial community embedded in a protective extracellular matrix. The biofilm’s structural organization allows bacteria to communicate, exchange genetic material, and resist both antimicrobial agents and innate immune responses, making early mechanical disruption essential for disease prevention [2].
If plaque is not removed, it undergoes mineralization through the deposition of calcium salts present in saliva, forming calculus (tartar). Its rough surface facilitates further plaque accumulation and deepens gingival inflammation [3].
The earliest clinical manifestation of periodontal disease is gingivitis, characterized by erythema, edema, and bleeding of the gingiva. At this stage, inflammation is confined to the soft tissues and is fully reversible with appropriate intervention. However, if gingivitis is allowed to persist, the inflammatory process extends deeper into the periodontal ligament and alveolar bone, leading to irreversible attachment loss. This marks the transition to periodontitis; a destructive condition defined by pocket formation, bone resorption, and eventual tooth mobility.
Once structural support is compromised, the disease cannot be reversed, and treatment focuses on halting further deterioration rather than restoring lost tissues [4].
Diagnostic Standards as the Foundation of Effective Treatment
Accurate diagnosis is the cornerstone of gold-standard periodontal therapy, and it requires a comprehensive oral health assessment (COHAT) performed under general anesthesia. Awake examinations, while useful for preliminary screening, cannot provide the level of detail necessary for definitive diagnosis. Anesthetized evaluation allows for proper inspection of all oral structures, precise periodontal probing, and -most critically- full-mouth intraoral radiography.
Radiographs are indispensable because a significant proportion of periodontal pathology occurs below the gingival margin and is therefore invisible during visual examination alone. Studies have demonstrated that more than 25% of dogs and nearly 50% of cats exhibit clinically important radiographic findings that would have gone undetected without imaging [5]. Radiographs reveal the extent of bone loss, the presence of endodontic lesions, retained roots, and other abnormalities that directly influence treatment planning.
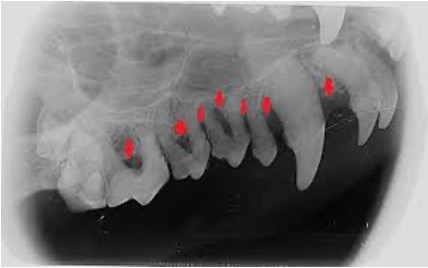
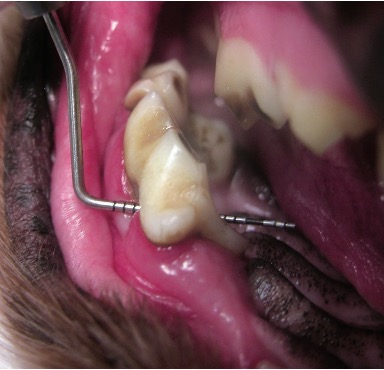
Periodontal probing (Fig1) complements radiographic assessment by quantifying pocket depths and identifying areas of attachment loss. In dogs, probing depths exceeding 4-5 millimeters typically indicate pathological pocketing, while in cats, even 1-2 millimeters may be significant due to species-specific anatomical differences.

Together, probing and radiography form the diagnostic foundation upon which all subsequent therapeutic decisions are based.
Gold-Standard Therapeutic Protocols
The gold-standard treatment of periodontal disease is a multi-step process that begins with professional mechanical debridement.
- Supragingival and Subgingival Scaling
Supragingival scaling removes visible plaque and calculus, but it is the subgingival cleaning that has the true therapeutic intervention.
Because periodontal disease originates below the gumline, thorough subgingival debridement is essential for removing biofilm, calculus, and necrotic cementum from root surfaces.
This process reduces bacterial load, resolves inflammation and creates an environment conducive to tissue healing.
- Root Planing
Root planing is a specialized procedure aiming for cleaning tooth roots below the gumline. It involves removing tartar, plaque, and diseased cementum using manual curettes (Gracey Curette) or ultrasonic scalers, reducing pocket depth, and smoothing root surfaces to promote gum reattachment and further refines the root surface, smoothing microscopic irregularities that might otherwise promote bacterial adherence, using a Gracey Curette.

- Polishing
Once scaling and root planing are complete, polishing is performed to eliminate micro-abrasions created during instrumentation, thereby reducing future plaque accumulation [1].
- Open Flap Debridement
In cases where periodontal pockets are too deep or complex to be adequately treated through closed (non-surgical) procedures, periodontal surgery becomes necessary.
Open-flap debridement allows direct visualization of root surfaces and alveolar bone, enabling the clinician to remove calculus and granulation tissue that would otherwise remain inaccessible. This technique is particularly valuable in the management of vertical bone defects and advanced furcation involvement.
- Guided Tissue Regeneration (GTR)
Guided Tissue Regeneration (GTR) is a technique performed to promote osseous regeneration, allowing for tissue growth (bone and soft tissues) to replace an infrabony periodontal pocket (a site of vertical bone loss).
This involves cleaning the infrabony pocket using hand curettes; potentially with a specialized ultrasonic curette if available.
A bone graft, along with a barrier membrane, is placed into the pocket, followed by tight closure of the gingival collar. GTR is performed to preserve structural integrity in cases of vertical bone loss. In select cases, guided tissue regeneration (GTR) may be employed to encourage the regrowth of periodontal ligament and bone.
Although GTR is not universally applicable, it has shown promising results in dogs with specific defect morphologies, particularly those with three-walled vertical defects that provide a natural containment structure for regenerative materials [6].
- Tooth Extraction
When periodontal destruction is severe and the prognosis for a tooth is poor, extraction becomes the most humane and effective treatment.
Teeth exhibiting advanced mobility, severe bone loss, or grade-three furcation exposure are unlikely to respond to conservative therapy.
Extraction eliminates the source of chronic infection and pain, preventing further systemic impact and improving the animal’s overall quality of life.
The AAHA guidelines emphasize that extraction should not be viewed as a failure of treatment but rather as an essential component of comprehensive periodontal care when indicated [1].
- Adjunctive Therapies
Adjunctive therapies may support periodontal treatment but should never replace mechanical debridement.
Local antimicrobial agents, such as doxycycline and chlorhexidine gels or clindamycin microspheres can be beneficial in reducing pocket depth in select cases.
Systemic antibiotics, however, are not routinely recommended and should be reserved for patients with systemic illness, osteomyelitis, or severe soft-tissue infection.
Overuse of antibiotics contributes to antimicrobial resistance and offers little benefit in the absence of systemic involvement [7].
Pain management is another critical aspect of periodontal therapy, as many animals experience significant discomfort both before and after treatment.
Multimodal analgesia, including Non-Steroidal Anti-inflammatory (NSAIDs)and local nerve blocks, ensures patient comfort and facilitates recovery.
The Role of Home Care in Long-Term Disease Control
Periodontal disease is a chronic condition that requires lifelong management.
Even the most thorough professional treatment cannot prevent recurrence if plaque is allowed to accumulate.
Daily tooth brushing remains the gold standard for home care, as it mechanically disrupts biofilm before it can mature. For owners unable to brush their pets’ teeth consistently, products approved by the Veterinary Oral Health Council (VOHC) offer scientifically validated alternatives that reduce plaque and calculus accumulation. Dental diets, chews, water/food additives, and oral gels can all contribute to maintaining oral health.

Conclusion
The gold-standard treatment of periodontal disease in dogs and cats is a comprehensive, evidence-based approach that integrates accurate diagnosis, mechanical debridement, surgical intervention when necessary, extraction of non-salvageable teeth, and lifelong home care.
This multimodal strategy is the only scientifically validated method for halting disease progression, alleviating pain, and improving systemic health outcomes in companion animals.
As veterinary professionals, our role extends beyond treating visible disease; towards educating clients, advocating for preventive care and ensuring that every patient receives the highest standard of oral health management.
References
- American Animal Hospital Association (AAHA). 2019 Dental Care Guidelines for Dogs and Cats.
- Marsh PD. Dental plaque as a biofilm and a microbial community. BMC Oral Health.
- Logan EI, Boyce EN. Oral health in companion animals. J Vet Dent.
- Arzi B, et al. Pathophysiology of periodontal disease in small animals. Vet Clin North Am Small Anim Pract.
- Verstraete FJM. Diagnostic value of dental radiography in dogs and cats. J Vet Dent.
- Smith MM, et al. Guided tissue regeneration in veterinary dentistry. Vet Surg.
- AVDC Position Statement on Antibiotic Use in Dentistry.
- Veterinary Oral Health Council (VOHC). Accepted Products for Plaque and Calculus Control.
- vet.cornell.edu/departments-centers-and-institutes/riney-canine-health-center/healt
- Hand Instruments – Canine & Feline – Curettes – iM3 USA | The Global Name in Veterinary Dentistry
- drvet.com.au articles. what-is-periodontal-disease
- im3vet.com. periodontal-probe-explorer-15-mm-standard